21 October 2021
Vancouver, BC – A study recently released in the medical journal Critical Care Medicine estimates that BC’s health care system prevented 1,153 people from acquiring sepsis in hospital or dying from the disease during a recent five-year period. The study also estimates that doing so saved the health care system and patients’ families approximately $51 million.
From 2014-18, work to improve sepsis care was led by the BC Patient Safety & Quality Council (the Council) and put into action by hundreds of clinicians across the province united through its BC Sepsis Network. The study’s authors estimate that during those five years:
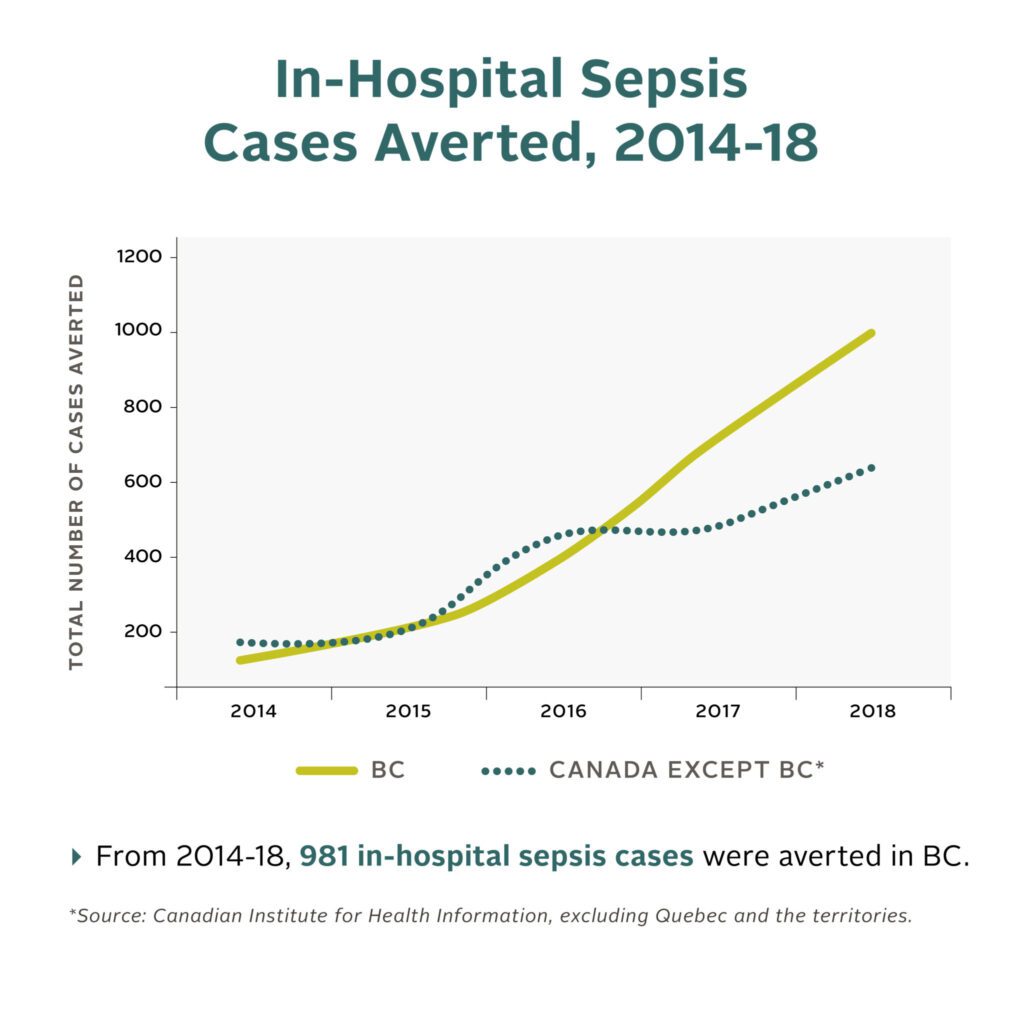
- 981 people were prevented from acquiring sepsis while in hospitals
- 172 people were prevented from dying from sepsis
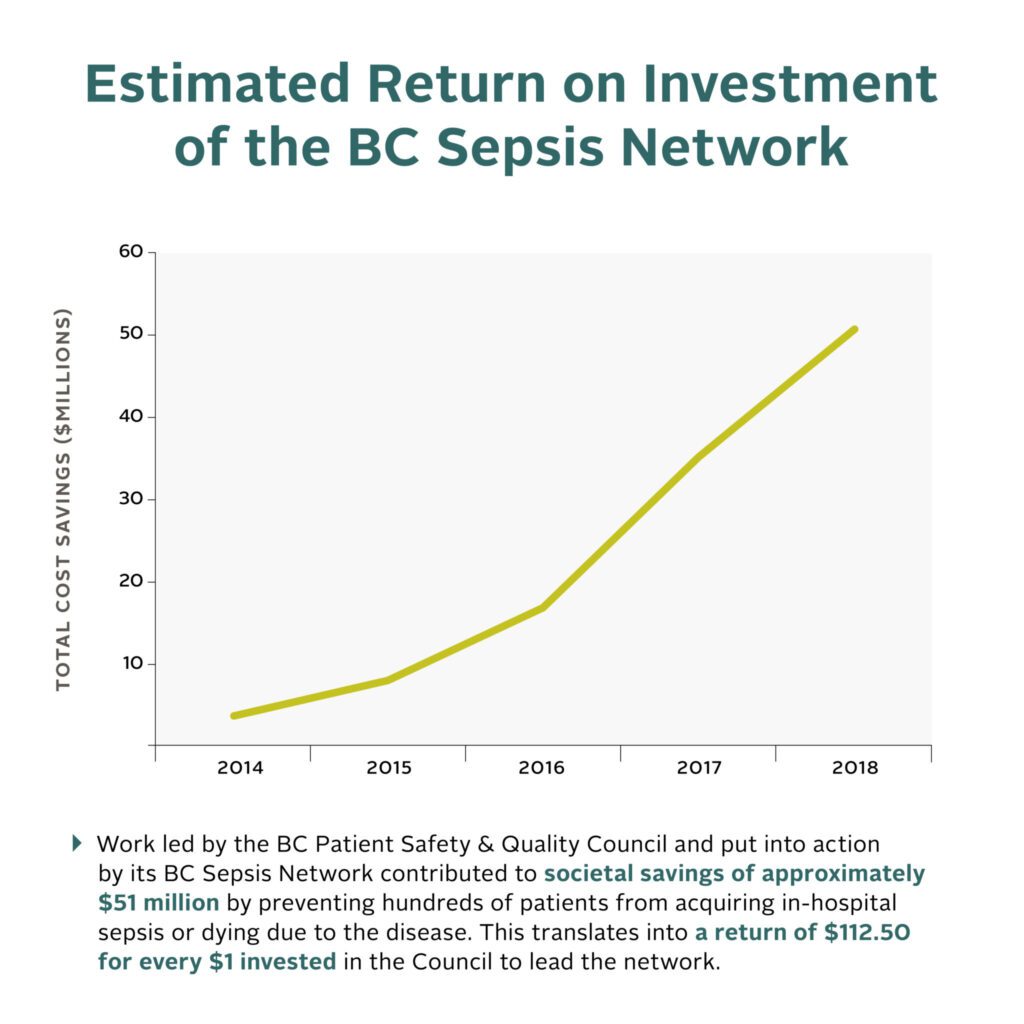
- A reduction of cases and deaths contributed to societal savings of approximately $51 million, including $49 million in savings for the health care system
- Every $1 invested by the Ministry of Health into the Council to lead this work resulted in $112.50 in savings to the health care system
Sepsis is a life-threatening condition that occurs when the body’s response to an infection becomes too severe. Each year, 30,000 Canadians are hospitalized because of sepsis – more than 30% of whom die – and the disease represents close to 20% of all global deaths.
Significant improvements in the quality of sepsis care can be seen since 2012 when the Council created the BC Sepsis Network to mobilize collective action. The network now includes more than 300 members from 36 hospitals who the Council brings together to focus on identifying and treating new infections early, preventing sepsis from developing as well as treating sepsis and septic shock. This new research shows the impact of targeting improvement work on a specific area of care and the Council’s unique expertise to lead that work by:
- Developing evidence-informed guidelines to improve early recognition and treatment of sepsis
- Sharing clinical best practice as new evidence is published locally and internationally, and supporting its implementation
- Accelerating the spread of treatment protocols through province-wide campaigns and education
- Building an active network of clinicians from across the province and supporting them to champion sepsis improvement within their organizations
- Engaging patients and families to inform where and how to focus improvement work
- Identifying new ways to leverage real-time data from intensive care and high acuity units to recognize emerging improvement priorities
- Improving teamwork and communication between point-of-care staff
Using screening tools, clinicians were able to identify patients early in the emergency department and, on hospital wards, those that had severe infections, sepsis and septic shock. The Council created new protocols for use that ensured rapid diagnostic tests were performed and timely therapies were delivered that have been shown to reduce the morbidity and mortality associated with sepsis. These therapies include the delivery of broad-spectrum intravenous antibiotics, rapid intravenous fluid administration and controlling the source of the infection. The final stage of these protocols is to ensure that at-risk patients are monitored closely for deterioration and cared for in an appropriate setting.
“Since we began focusing on improving care for sepsis, BC has gone from being one of the lowest-performing provinces to leading the way,” said Dr. Devin Harris, Chair of the BC Patient Safety & Quality Council and an emergency department physician. “And now we can see the impact of that work: more than 1,150 families did not have to see their loved ones acquire sepsis, or worse, die from the disease.”
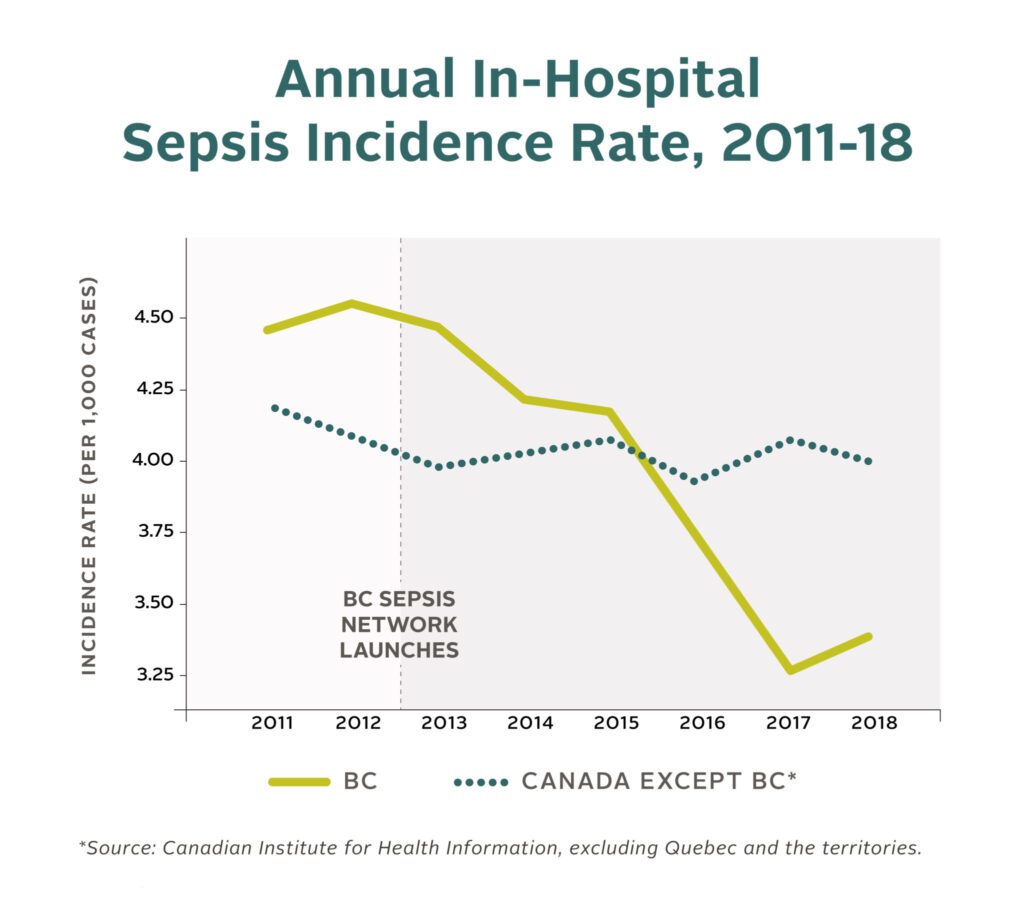
This study – one of the first of its kind – estimates the degree to which care for sepsis has improved in BC as well as how the province compares to the rest of the Canada when it comes to preventing and treating sepsis. BC outperformed the rest of the country in every metric examined in the study – for example, the in-hospital sepsis caseload decreased by 17% in BC compared to 1.7% in the rest of Canada by the end of 2018 (excluding Quebec and the territories).
“These results show what can happen when clinicians who are passionate about improving the quality of care they provide are brought together and supported to lead that work within their organizations,” said Dr. David Sweet, the Council’s Provincial Clinical Lead for Sepsis and a critical care physician, “I’m so proud of our sepsis network members whose hard work has made such an impact for British Columbians and transformed our province into a national and global leader in caring for sepsis.”
Quick Facts
The BC Patient Safety & Quality Council receives its mandate from the Minister of Health to:
- Bring system-wide leadership and co-ordination in advancing a culture of quality within the province;
- Facilitate the building of capability and expertise for patient safety and quality in the BC health system;
- Support health authorities and other health sector stakeholders in their continuing efforts to improve quality;
- Improve health system transparency and accountability to patients and the public for the safety and quality of care provided in BC; and
- Identify and promote local, regional and provincial opportunities for engaging the patient perspective in health care transformation.
Study Abstract
Objectives: Sepsis is a life-threatening medical emergency. There is a paucity of information on whether quality improvement (QI) approaches reduce the in-hospital sepsis caseload or save lives and decrease the healthcare system and society’s cost at the provincial/national levels. This study aimed to assess the outcomes and economic impact of a province-wide QI initiative in Canadian.
Design: Retrospective population-based study and return on investment analysis.
Setting: The sepsis cases and deaths averted over time for British Columbia (BC) were calculated and compared to the rest of Canada (excluding Quebec and three territories).
Patients: Aggregate data were obtained from the Canadian Institute for Health Information on risk-adjusted in-hospital sepsis rates and sepsis mortality in acute care sites across Canada.
Interventions: In 2012, the British Columbia Sepsis Network (BCSN) was formed to reduce sepsis incidence and mortality through education, knowledge translation and quality improvement (QI).
Measurements and Main Results: A return on investment (ROI) analysis compared the financial investment for the BCSN to the savings from averted sepsis incidence and mortality. An estimated 981 sepsis cases and 172 deaths were averted in the post-BCSN period (2014 to 2018). The total cost, including the development and implementation of BCSN, was $449,962. Net savings due to cases averted after program costs were considered was over $50 million in 2018. This translates into a return of $112.5 for every dollar invested.
Conclusions: BCSN appears to have averted a greater number of sepsis cases and deaths in BC than the national average and yielded a positive ROI. Our findings strengthen the policy argument for targeted QI initiatives for sepsis care and provide a model of care for other provinces in Canada and elsewhere globally.
Media Assets